Nick TriggleHealth correspondent

 PA Media
PA Media
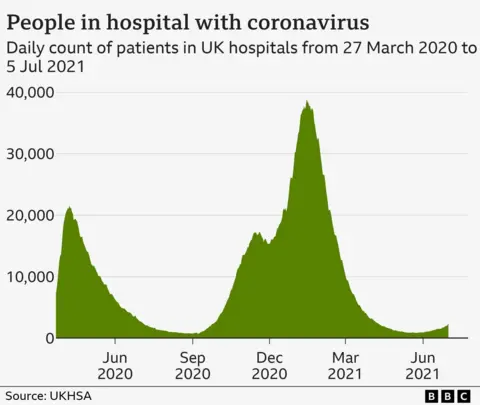
Patients were harmed as the NHS was on the brink of collapse in the UK during the pandemic, the Covid inquiry says.
It described staff working in "war zones" and patients not getting the care they needed as hospitals and ambulances struggled to cope with the surge in Covid.
The inquiry also criticised the weak state the NHS entered the pandemic in and suggested the Stay Home, Protect the NHS, Save Lives slogan may have caused harm by deterring those with other health problems from seeking help.
Inquiry chair Baroness Hallett said: "We coped, but only just. Collapse was only narrowly avoided thanks to the extraordinary efforts of all those working in health care."
To cope with another pandemic there had to be greater capacity to scale-up hospital and ambulance services, according to the inquiry.
Almost 227,000 people died from Covid in the UK between March 2020 and May 2023, when the World Health Organization said the "global health emergency" was over.
Across more than 400 pages, the report describes how the NHS faced intolerable pressure as it faced wave after wave of Covid.
- Waiting times for ambulances, even for the most life-threatening calls, grew with some services turning to the military to help
- The NHS struggled to cope with the surge in Covid patients, particularly in the first wave, with supplies of oxygen almost running out in places
- Intensive care staffing ratios were diluted, going from one nurse to one patient to one to four at times
- Covid patients faced long delays for the NHS 111 service and ambulances
- Disruption to cancer screening and a drop in people coming forward with signs of the disease led to missed and delayed diagnoses, which cost lives
The report highlighted how there was a decline in attendances to A&E and other settings for non-Covid emergencies, including heart attacks, suggesting the slogan Stay Home, Protect the NHS, Save Lives inadvertently sent the message health care was closed.
And it said the cancellation en masse of non-urgent care, such as knee and hip replacements, had a "debilitating effect" on patients' lives and mobility.
Tough restrictions should be avoided
Visiting restrictions meant some vulnerable patients, including women giving birth and people with disabilities, were left without vital support – and such tough rules needed to be avoided if possible in the future, the inquiry said.
The restrictions also left bereaved family members heartbroken, guilty and angry as their loved ones died along.
The report also criticised:
- Inappropriate do not resuscitate orders imposed on groups of people, including those with learning disabilities and older people
- "Flawed" infection control guidance at the start that failed to recognise the virus could also be spread in the air
- Shortages of personal protective equipment (PPE) such as masks, gloves and gowns meant that doctors and nurses had to work in "inadequate" conditions that put them at risk
It said supply levels of of PPE got "dangerously low" – the inquiry was told at one point the NHS was just days away from running out of key items.
Staff were left with with post-traumatic stress disorder after working in what some described as "war zones", it added.

Dr Tom Dolphin, of the British Medical Association, said the failings meant that many staff "tragically paid with their lives". Research has shown health workers had higher excess mortality in the first year of the pandemic than other workers.
He said this had disproportionately affected those from ethnic minorities.
"The impact on doctors and our colleagues was stark, as painfully recounted in this report," Dolphin added.
And he said the NHS remained "over-stretched" and "under-staffed" to this day.
The Covid-19 Bereaved Families for Justice said the report was "utterly damning".
"Our loved ones, many of whom where healthcare workers themselves, paid with their lives.
"Years of austerity left the NHS dangerously exposed, without the staff, beds or resilience needed to withstand a major shock."
Layla McKay, of NHS Confederation and NHS Providers, which represents hospitals, said: "It is vital that these lessons translate into meaningful action, strengthened preparedness and a more resilient health and care system for the future."

 German (DE)
German (DE)  English (US)
English (US)  Spanish (ES)
Spanish (ES)  French (FR)
French (FR)  Hindi (IN)
Hindi (IN)  Italian (IT)
Italian (IT)  Russian (RU)
Russian (RU)  3 weeks ago
3 weeks ago




















Comments